Breast Reconstruction Surgeon Bakersfield and Orange Co
Breast Reconstruction Surgery in Southern CA
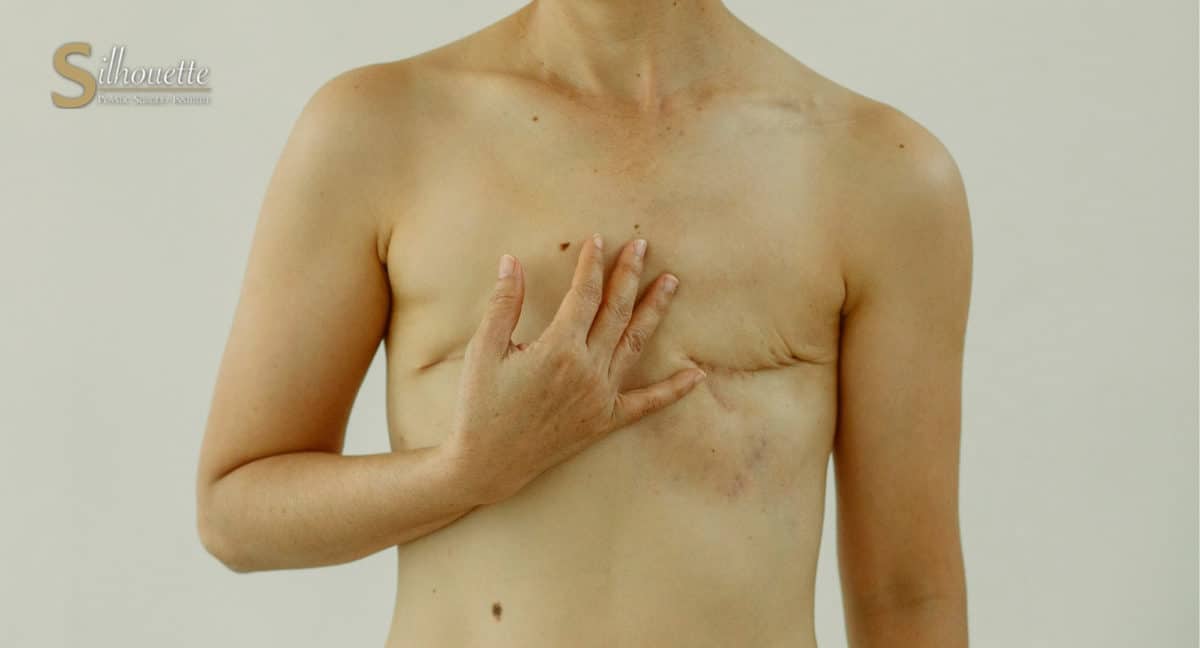
Reconstruction of a breast that has been removed due to cancer or other disease is one of the most rewarding surgical procedures available today. New medical techniques and devices have made it possible for surgeons to create a breast that can closely match a natural breast in form and appearance. Breast reconstruction surgery is often possible immediately following a mastectomy, so the patient wakes up with a breast mound already in place, having been spared the experience of seeing herself with no breast at all.
But bear in mind that post-mastectomy breast reconstruction is not a simple procedure. There are often many options to consider as you and your doctor explore what’s best for you. The following information about breast reconstruction surgery will give you a basic understanding of the entire process — when this surgery is appropriate, how it’s done, and what kind of results you can expect. To schedule a consultation with board-certified plastic surgeon Dr. Daneshmand, call 949-359-8397 today.
What is a Breast Reconstruction?
Breast reconstruction surgery is designed to completely recreate one or both breasts following breast cancer treatment. There are many types of breast reconstruction, but oftentimes they require multiple surgeries. Breast cancer survivors may choose an immediate reconstruction – which is a reconstruction that occurs right after breast cancer surgery – or a delayed reconstruction – which is a reconstruction that occurs months or years after cancer treatment.
What is a Mastectomy?
A mastectomy is a surgical procedure that removes some or all of a woman’s breast tissue in order to fight breast cancer.
Learn more about our Bakersfield breast cancer reconstruction surgery options.
Common Reasons Why Women Undergo Breast Reconstructions
The most common reason why women undergo breast reconstruction surgery is that they had a mastectomy. Aside from missing one or both breasts due to this surgery, a woman may also choose a breast reconstruction because she:
- Wants to feel confident in her body and her breast shape
- Wants her chest to look normal, balanced, and symmetrical
- Doesn’t want to wear an external prosthesis every day, which is a breast form that fits inside a bra
- Wants her clothes to fit correctly on her chest
Types of Breast Reconstruction
In this day and age, there are many types of breast reconstruction techniques out there, the most common ones being breast implant-based reconstruction and tissue flap reconstruction. The type of breast reconstruction that is best for you will depend on your body fat and the amount of breast tissue you have leftover.
Breast Implants
Breast implant reconstruction will use saline, silicone, or gummy bear implants. There are many ways to do this. A surgeon may choose to put the implant under the chest muscle or on top of the chest muscle. Some breast surgeons use breast implants along with tissue expanders. If you choose this method, you will receive the expander first. Every week or two, your surgeon will slowly inject saline into the expander. This process allows your breast skin to stretch slowly and comfortably following a mastectomy. Finally, your surgeon will insert a breast implant.
Tissue Flap Procedures
Tissue flap reconstruction is much more complicated than breast implant reconstruction. The point of tissue flap surgery is to completely rebuild the breast(s) from tissue on other parts of your body.
- Transverse Rectus Abdominis Muscle (TRAM) Flap Reconstruction uses skin, fat, and muscle from the lower abdomen to create one or two new breasts. The tissue used during TRAM flap procedures stays connected to its original abdominal blood supply.
- Deep Inferior Epigastric Perforator (DIEP) Flap Reconstruction also uses abdominal tissue to recreate one or both breasts. The difference here is that this flap procedure doesn’t use abdominal muscle, only the skin and fat. Additionally, plastic surgeons must connect this tissue to a new blood supply in the chest wall.
- Profunda Artery Perforator (PAP) Flap Reconstruction creates one or two breasts using tissue from the patient’s upper inner thigh. Surgeons do not use thigh muscles during this breast reconstruction method.
- Transverse Upper Gracilis (TUG) Flap Reconstruction is similar to the PAP flap in that it requires tissue from the patient’s upper inner thigh. The main difference here is that this procedure requires thigh muscle.
- Latissimus Dorsi (LD) Flap Reconstruction uses fat, skin, and muscle from the upper back in order to create one or two breasts. Sometimes plastic surgeons use this procedure in conjunction with breast implants to create the most natural breasts possible.
- Inferior Gluteal Artery Perforator (IGAP) and Superior Gluteal Artery Perforator (SGAP) Flap Reconstruction recreate one or both breasts with tissue from the butt.
Flap Procedure Risks
Autologous tissue reconstruction comes with several risks, including:
- The donor tissue can get larger or smaller during weight fluctuations
- Healing can take longer than implant surgery because there are basically two sections of your body that a surgeon operates on: the tissue donor section and the breasts
- If your surgeon uses muscle for an autologous tissue reconstruction, the donor site will likely feel and function differently once it heals
- Hernia at the donor site
- Blood clots
- Donor tissue death due to damaged blood vessels
- Infection
- Noticeable scarring
- Anesthesia complications
Nipple-Areolar Reconstruction
Dr. Daneshmand usually performs nipple and areola reconstruction as the final procedure. Dr. Daneshmand will use local tissue flaps for nipple reconstruction. To recreate the areola, plastic surgeons may use a tattoo or a skin graft. If the areola is reconstructed with a skin graft, the graft itself may heal with enough pigmentation to simulate a natural areola. If not, a simple tattoo can recreate a natural areola color.
What is a Nipple Sparing Mastectomy?
In some cases, surgeons will remove all breast tissue except the nipple and areola. So when it comes time for nipple reconstruction, plastic surgeons can just use the natural nipple-areola complex for the most natural look.
Opposite Breast Surgery
If you only have cancer in one breast, that means you’ll need a reconstruction in only one breast. For the sake of symmetry, many women also have to undergo opposite breast surgery. This could include a breast lift or a breast reduction surgery to ensure that the natural breast matches the size and shape of the reconstructed one.
Does Breast Reconstruction Affect My Risk of Breast Cancer Recurrence?
Breast reconstruction does not affect breast cancer recurrence according to the American Cancer Society. If your cancer does come back, it’s likely unrelated to your breast reconstruction. Your breast surgeon may recommend periodic mammograms on both the reconstructed breast and the other breast. If your reconstruction involves an implant, be sure to go to a radiology center where technicians are experienced in getting reliable x-rays of a breast reconstructed with an implant.
Can I Undergo a Breast Reconstruction During Chemotherapy?
Yes, technically you can undergo breast reconstruction during radiation therapy, although this isn’t always recommended by doctors. Radiation treatment is violent on the body just like reconstructive surgery. Some women aren’t physically and mentally capable of handling both chemotherapy and the pain associated with healing from major surgery at the same time. But every woman and situation is different. Most women opt for immediate reconstruction, which sometimes means they’re healing from their surgery and receiving chemotherapy at the same time. Or, in another scenario, some women get part of their reconstruction done immediately and then finish the rest of their reconstruction once they’ve completed chemotherapy.
For many women undergoing radiation treatment, delayed reconstruction is the best option. This is because chemotherapy after a reconstruction can change the shape, color, texture, and appearance of the reconstructed breast(s). This is especially the case with women who have a permanent implant. In fact, some research even suggests that the breast reconstruction process can interfere with chemotherapy effectiveness, according to BreastCancer.org.
Be sure to discuss your reconstruction timeline with your plastic surgeon. They will help you determine when is the best time to undergo this surgery, especially if you’re enduring chemotherapy.
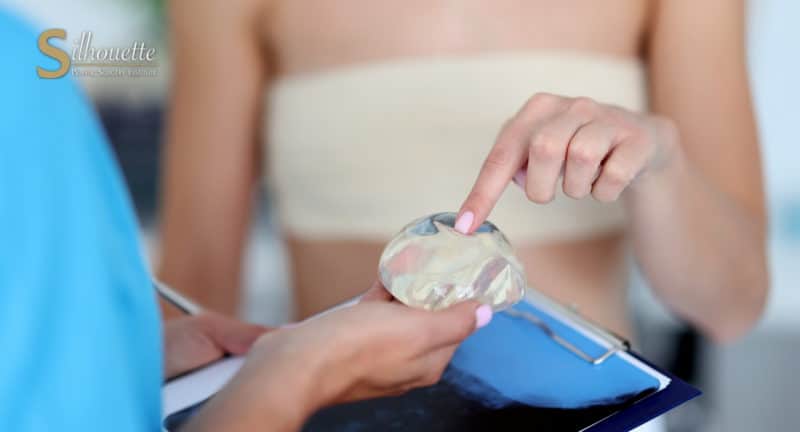
How Long Do Breast Implants Last?
According to the American Society of Plastic Surgeons, breast implants can last anywhere from 10 to 20 years. But if you experience capsular contracture, rupture, rippling, and other implant issues, you will have to undergo breast revision surgery to fix them.
Are Silicone Implants Better Than Saline Implants?
Many reconstructive surgery patients opt for silicone implants because they feel more natural than saline.
Anatomic vs. Round Implants
Teardrop or anatomic implants were introduced to better simulate the natural contour of the breast. Many surgeons like these implants and use them both for breast reconstruction and breast augmentation. Dr. Daneshmand typically uses round implants, but he occasionally uses anatomic implants as well. One of the disadvantages associated with contoured implants is that they are textured. In the saline-inflatable implants, this sometimes means that they will be more palpable, they may have a higher rate of rupture, and there may be more visible rippling.
Do Breast Implants Cause Cancer?
There is no evidence that the presence of breast implants causes breast cancer or increases your risk of getting breast cancer. However, the FDA has identified a possible link between breast implants and anaplastic large cell lymphoma (ALCL) and breast implant-associated squamous cell carcinoma (BIA-SCC) according to the Mayo Clinic. In fact, this immune system cancer is often called breast implant-associated anaplastic large cell lymphoma (BIA-ALCL). It’s important to note that the limited research conducted so far indicates that textured breast implants don’t cause ALCL, instead it just raises the cancer risk.
Can You Get a Mammogram With Breast Implants?
If you’re a breast cancer survivor, you must get regular mammograms even if you have breast implants. For women who have never had breast cancer, it’s crucial to get regular screenings starting at age 40 according to the American Cancer Society. If you have breast implants, be sure to tell the mammogram technologist before they start the scan.
Do Plastic Surgeons Perform Mastectomies?
Generally, the plastic surgeon works with a general surgeon during breast reconstruction surgery. Dr. Daneshmand has extensive experience in working with general surgeons in order to give breast cancer survivors the best looking and feeling set of breasts after their health crisis.
How Many Surgeries Are Required for Breast Reconstructions?
Breast reconstruction usually involves multiple operations. The first stage, whether done at the same time as the mastectomy or later on, is usually performed in a hospital. Follow-up procedures are usually performed in an outpatient facility.
Generally, the initial reconstructive operation is the most complex. Follow-up surgery may be required to replace a tissue expander with an implant or to reconstruct the nipple and the areola. Many surgeons recommend an additional operation to enlarge, reduce, or lift the natural breast to match the reconstructed breast.
Does Health Insurance Cover Breast Reconstruction Surgery?
Most health insurance companies don’t cover plastic surgeries because they’re generally considered elective procedures that aren’t medically necessary. However, breast reconstruction surgery is different. The Women’s Health and Cancer Rights Act (WHCRA) of 1998 requires most health insurance companies to cover breast reconstruction surgery for breast cancer survivors.
Call Silhouette Plastic Surgery Institute Today
If you were recently diagnosed with breast cancer and you’re looking for the best Orange County plastic surgeon to complete your mastectomy and breast reconstruction, look no further. Dr. Daneshmand at Silhouette Plastic Surgery Institute has 30 years of experience in giving women the breasts and bodies of their dreams. He can do the same for you. Call 949-359-8397 today to schedule a consultation.
Check out our breast reconstruction surgery before and after photos!
